Ultrasound-Guided PVA Workshop
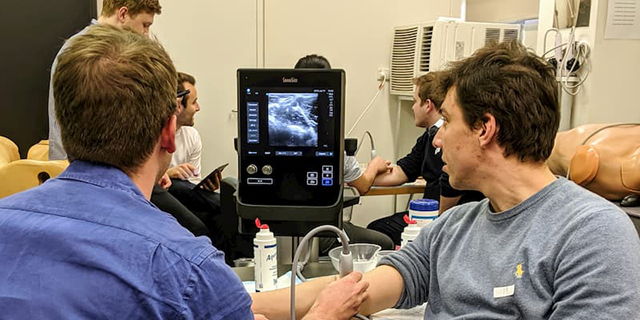
The University of Melbourne's Ultrasound Guided Peripheral Venous Access (PVA) Workshops, held on July 16, 17 and 23, were the largest held in the Southern Hemisphere.
The workshop targeted final year medical students to upskill on the use of ultrasound to help with PVA during their intern year, next year.
Students became equipped with the basic skills required to perform this procedure and were encouraged to return to practice for two weeks on ultrasound simulators to further enhance their skills.
The workshop covered using ultrasound to guide inserting an "IV" (intravenous) catheter (a small plastic tube) into a peripheral vein on an arm or leg in order to take blood samples, administer drugs and/or fluids.
PVA is a very common procedure, performed by doctors, nurses, and paramedics, for adults and children.
It is performed pre-hospital by general practitioners, nurses and paramedics.
Finding a vein and inserting the catheter can be very difficult in some circumstances.
Commonly visible veins, on the back of the hand or front of the elbow, may not be available due to damage from previous use.
Veins can be invisible to the naked eye because of low blood pressure/dehydration, or other patient factors.
Children's veins can be particularly difficult when they are frightened or in pain.
Difficulty with PVA can cause pain and stress to the patient, and stress to the practitioner trying to get the catheter in, often due to multiple failed attempts.
It commonly leads to delay in drawing blood for tests, administering drugs including pain relief medications, intravenous fluids and antibiotics, and in obtaining advanced medical imaging such as CAT scans.
These contribute to delays in case management, discomfort, and dissatisfaction with service on the behalf of the patient.